CASE20210825_002
Complex Percutaneous Coronary Intervention with Impella Support in a High Risk Elderly Patient
By ,
Presenter
Su Hnin Hlaing
Authors
1, 1
Affiliation
, Australia1
Complex PCI - Calcified Lesion
Complex Percutaneous Coronary Intervention with Impella Support in a High Risk Elderly Patient
1, 1
, Australia1
Clinical Information
Patient initials or Identifier Number
Mr B.H
Relevant Clinical History and Physical Exam
89 year old independent man presented with NSTEMI on the background oflikely ischemic cardiomyopathy EF 30% with moderate mitral regurgitation andadmission with decompensated heart failure in 2020. Other comorbidities includechronic kidney disease stage 5, hypertension, urothelial cancer and rectalcancer. Initially managed medically and not for angiogram due to CKD but the patientpresented again with ongoing chest pain and significantly elevated cardiactroponin. Haemodynamically stable.
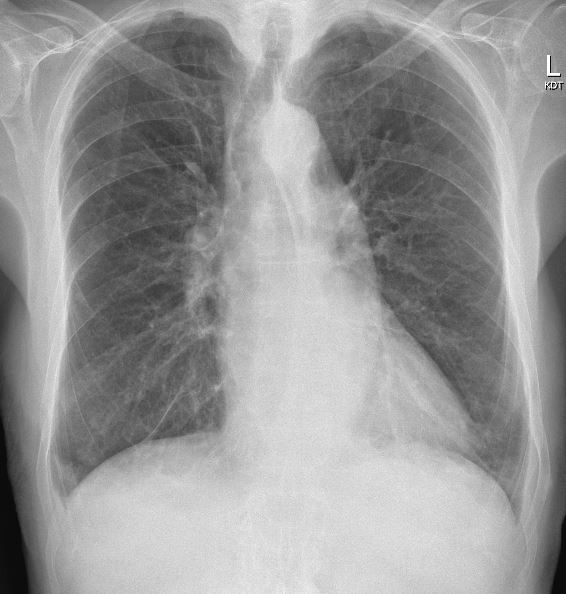
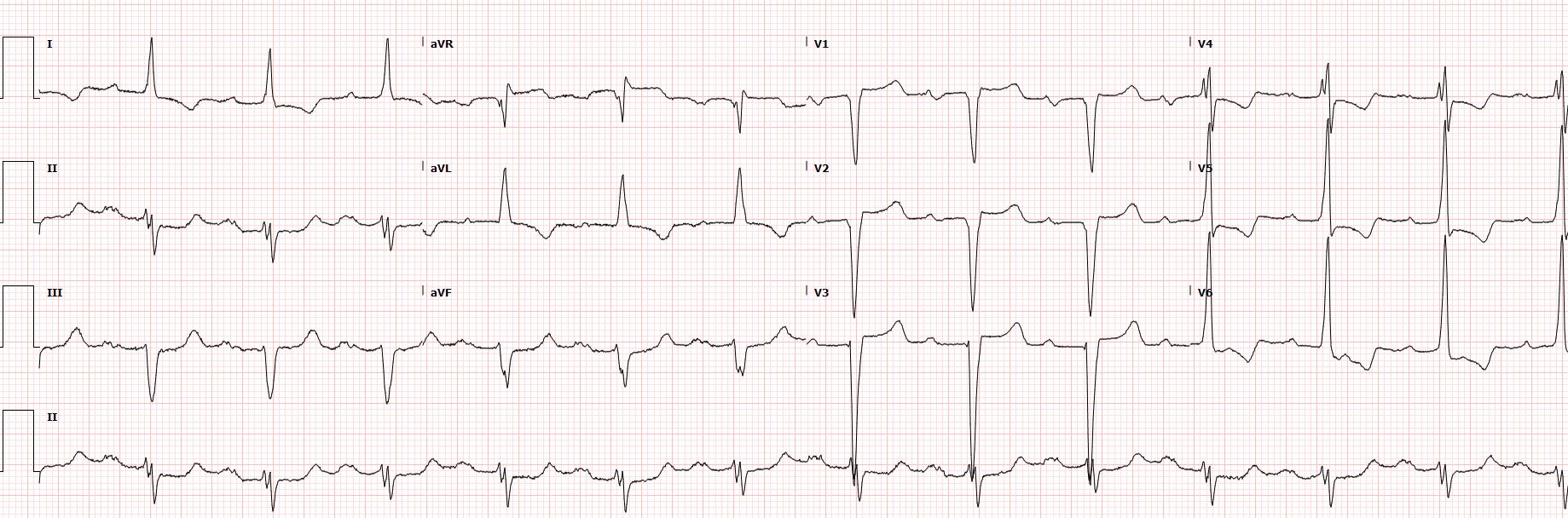
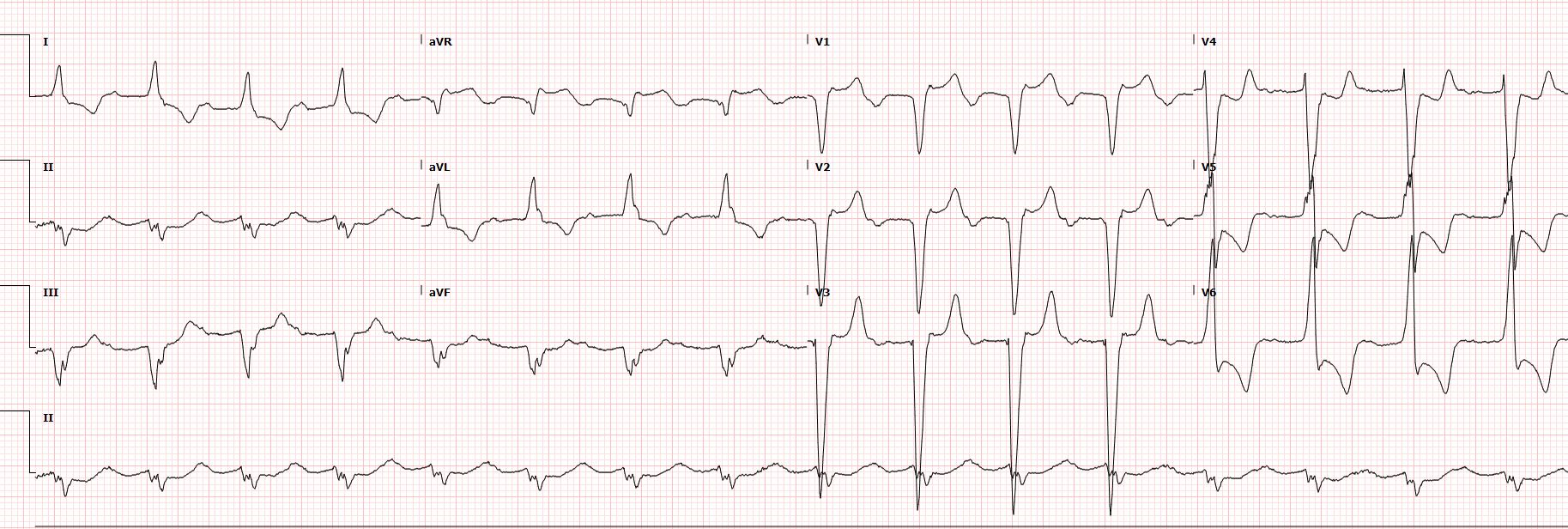



Relevant Test Results Prior to Catheterization
cTnI -35906 ng/L
 Pre PCI angio LCA.avi
Pre PCI angio LCA.avi
 Pre PCI angio RCA.avi
Pre PCI angio RCA.avi
Relevant Catheterization Findings
ImpellaCP assisted left main to mid LAD axis rotablation with 1.25,1.5,1.75 burrs and2.5mm intracoronary shockwave lithotripsy (IVL) was performed.IVUS guidedSynergy 3x 28 and 2.5 x 38 DES were inserted from mid LAD to ostial LM.Diagonal ostium treated with 2.5 IVL.Unable to wire severe calcified ostialleft cicrumflex disease.RCA was treated with Synergy 3.5 x 24 & 3 x48.Impella was weaned off at the end of the case. Patient has been pain free sinceand Creatinine improved to 272umol/l
 Rota 1.75.avi
Rota 1.75.avi
 Post stent angio LCA.avi
Post stent angio LCA.avi
 post stent angio RCA.avi
post stent angio RCA.avi
Interventional Management
Procedural Step
Impella CP was inserted via left femoral artery. Right radial artery was accessed with 8 Fr sheath. Using 6 Fr EBU 3.5 guide catheter, LCA was imaged with IVUS. Wired BMW and Corsair Pro was used . Rota 1.25 burr to prox LAD then used 1.75 burr to left main, then 1.5 burr again to proximal and mid LAD. Telescope 6Fr was also used. Predilated with NC 2.5 x12 but there was still a waste remaining. IVL catheter 2.5 x 12 was used and 6 x shockwaves delivered to left main and LAD and 1 shockwave delivered to diagonal. Unable to wire ostial LCx with Fielder XTR, Sion and Pilot 50 using hairpin technique and Sasuke microcatheter. Deployed DES Synergy 2.5 x 38 to mid LAD and Synergy 3 x 28 to proximal LAD to left main. Post dilated with NC 3 x 20, 3 x 12 and 3.5 x 12. Repeated IVUS after PCI. Using JR4 6Fr guided catheter and with IVUS guidance, RCA was predilated with NC 2x 12, NC 2.5 x 12 , NC 3x 12. Deployed DES Synergy 3 x 48 to mid RCA and 3.5 x 24 to proximal RCA. Post dilated with NC 3.5 x 12. Left cirumfex flow was unchanged in the end of the procedure and it also gets collaterals from RCA. During LM/LAD rota and during RCA PCI , patient was Impella-dependent. Impella was weaned off at the end of the procedure and patient was transferred to coronary care unit.
 Impella insertion .avi
Impella insertion .avi
 IVL left main.avi
IVL left main.avi
 Synergy 3 x 28 to LM to prox LAD.avi
Synergy 3 x 28 to LM to prox LAD.avi
Case Summary
Patient has been chest pain free since procedure. Patient did not require dialysis and renal function was slightly improved. During follow up, complained of lethargy and dyspnoea on exertion but no decompensated heart failure symptoms or chest pain. Repeat TTE showed EF unchanged and grade 2-3/4 MR on transesophageal echocardiogram. CRT-P was implanted 2 weeks ago. Patient was referred to structural heart team and will be monitored MR for consideration of mitraclip in the future. Patient is still independent with activities of daily living and still drives locally.
